A mole is a benign growth of pigment producing cells called melanocytes. Melanocytes are randomly distributed in cells in all 3 layers of the epidermis. The ratio of melanin distributed into each skin cell determines overall skin color. Current thinking is that moles form because melanocyte precursor stem cells known as melanoblasts, in utero, migrate along neurocutaneous paths, into moles under the epidermis, going to deeper layers, often following neuronal cells. This gives rise to deeper moles such as congenital birthmarks. In another mechanism, melanoblasts remain below these deeper tissue layers and do not migrate and remain dormant stem cells. These melanocyte precursor stem cells are stimulated by signals that cause them to grow into moles. This may occur shortly after their arrival in the skin or many years later. A sunburn can facilitate this process. Melanoma is a cancerous growth derived from abnormal melanocytes.
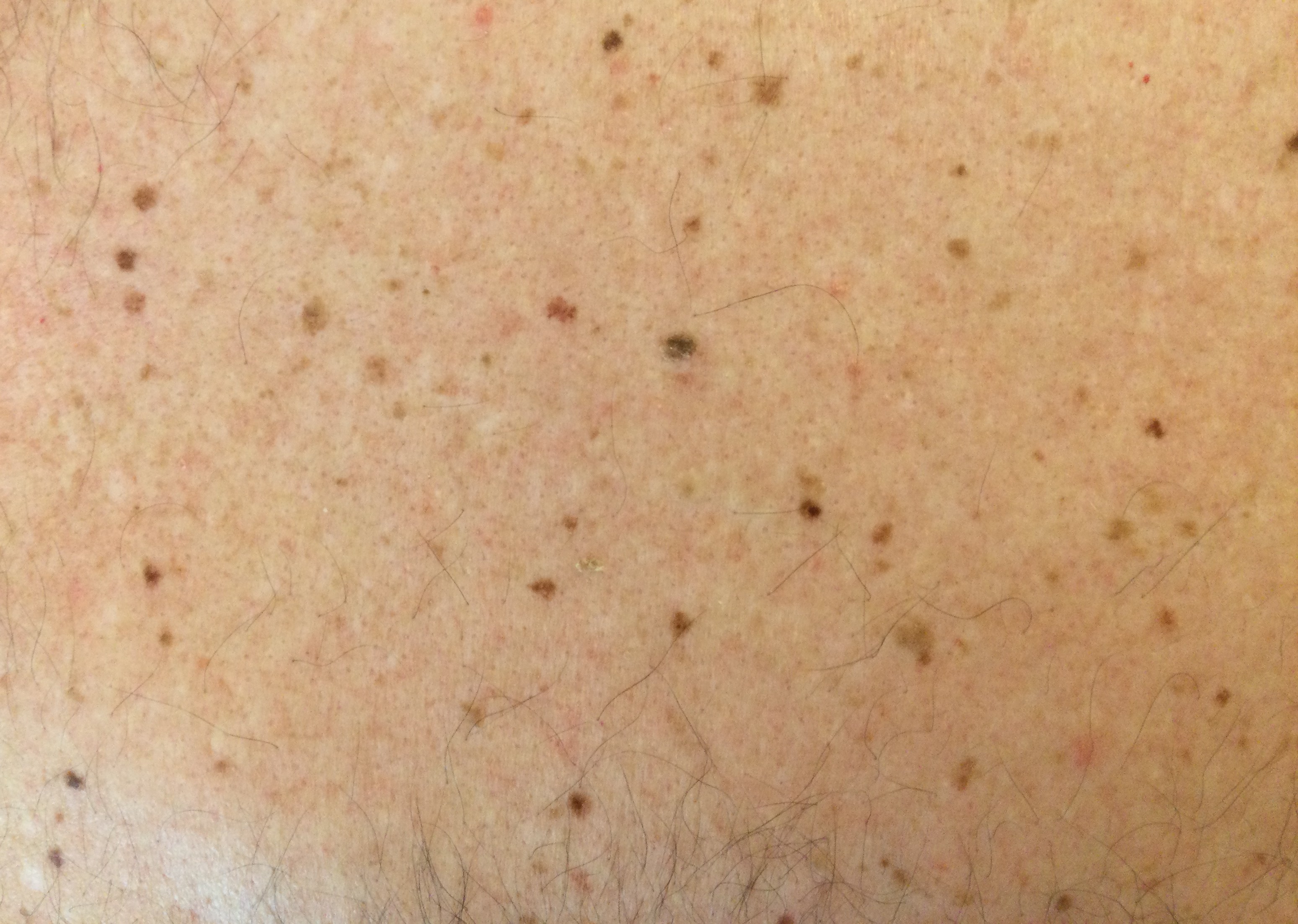
People with many moles have an increased risk of melanoma.
Melanoma Risk Factors
Moderate Risk:
- Total nevi greater than 40 but less than 60
- Lots of freckles
- 1-2 atypical moles
- Blue, hazel, green eye color
- Light brown hair
- Very fair skin, sunburns easily
- Greater than 5 blistering sunburns by age 20
High Risk:
- Total moles greater than 60 but less than 80
- 3-4 atypical moles
- Red hair
- Family history of melanoma in 1 or 2 first degree relatives
- Personal history of nonmelanoma skin cancer
- Tanning bed use
- Transplant recipient
Ultra-High Risk:
- Total moles greater than 100
- 5 or more atypical moles
- Personal history of melanoma in 3 or more relatives on the same side of the family
- Atypical cancers (leukemias)
- Xeroderma pigmentosum
- Rule of Three: Pancreatic cancer, astrocytoma, breast cancer, colon cancer, ovarian cancer, prostate cancer
- Consider genetic testing for mutations in genes associated with other melanoma-cancer syndromes
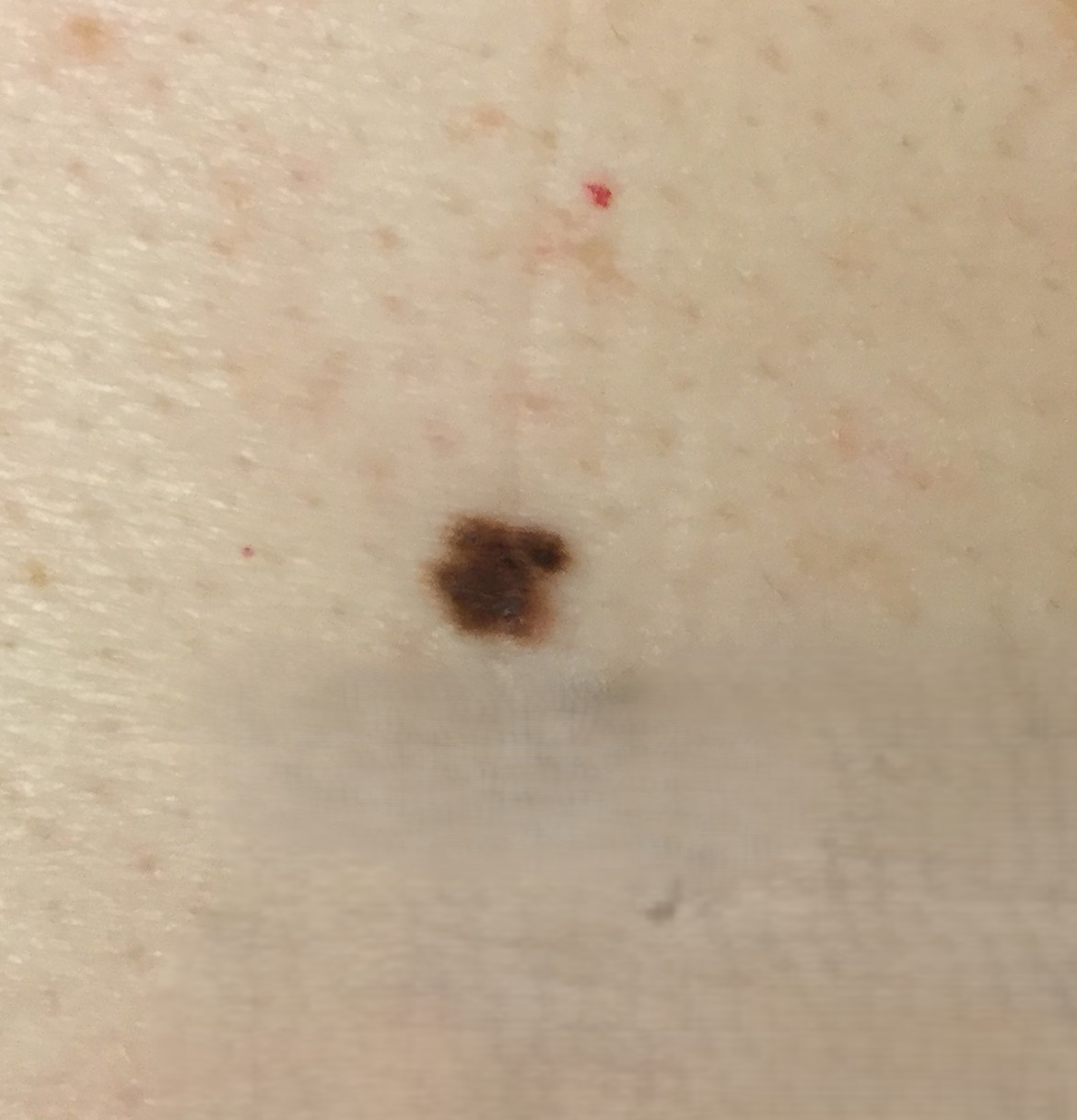
An Atypical Mole
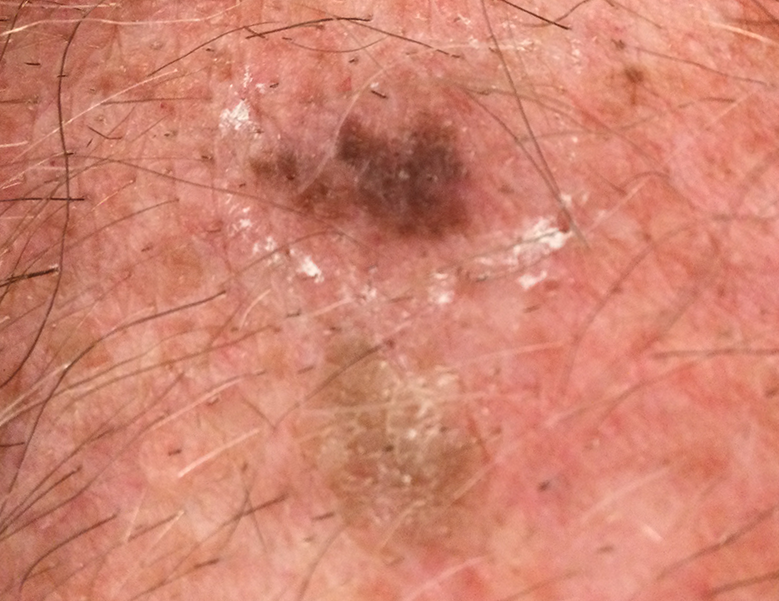
Melanoma
30% of the time a melanoma develops in a pre-existing mole. This means that most melanomas develop de novo. pigmented lesion. Numerous factors contribute to development of a melanoma. It is a complex interplay between genetic susceptibility, environmental risk factors (such as intermittent, intense ultraviolet radiation exposure), and epigenetic changes. UV radiation causes DNA mutations, produces reactive oxygen species that damage DNA in skin cells, stimulates immunosuppression in the skin, damages endonucleases, which are DNA repair enzymes, and inactivates p53 tumor suppressor gene, which regulates normal cell growth cycles in the skin. This creates the perfect setting for a melanoma to occur.
It is thought that patients with many moles are more prone to develop melanoma than those with fewer moles because only an initial dose of UV radiation is needed to cause melanocytes in these patients to grow and transform into melanoma without additional UV exposure.
Changing moles or growths on the skin should be evaluated and biopsied if indicated for diagnosis. Melanoma prognosis is closely linked with how deep the cancer has invaded the skin.
Excellent therapies are available for melanoma. In addition to surgical removal, combined immunotherapies have greatly improved survival for this disease.
A total body skin examination should be performed that includes the scalp, lips, mouth, genitals, buttocks and perianal area, hands and soles, and nails. Do not wear make-up, jewelry, or nail polish during your exam. The frequency of the exam depends on your risk of developing cancer, prior history of skin cancer and atypical moles, family history, and UV exposure.
Patients who are high risk for developing melanoma or who have had melanoma (s) should be seen more frequently, perhaps every 4-6 months so potentially concerning changes can be detected early.